You have probably seen ipamorelin grouped with CJC-1295 in fitness forums and anti-aging clinics — promoted as a "cleaner" growth-hormone booster that avoids the cortisol spike associated with older peptides like GHRP-2 and GHRP-6. The selectivity claim is real and supported by peer-reviewed data. The leap from "more selective in animal models" to "safe and effective for human use" is not. Ipamorelin is a research-stage peptide, not an approved drug — and the difference matters in ways the marketing rarely explains.
Summary / Quick Answer: What Is Ipamorelin and Does the Selectivity Claim Hold Up?
Ipamorelin is a synthetic five-amino-acid pentapeptide developed by Novo Nordisk in the 1990s. It stimulates growth hormone release by activating the ghrelin receptor (GHS-R1a) and, unlike older GHRPs, does not produce significant elevations in cortisol or prolactin at pharmacologically relevant doses — a distinction confirmed in animal studies. Human clinical trials for its original indication (post-operative ileus) were discontinued without regulatory approval. It is NOT FDA-approved for any use and is prohibited in competitive sport under WADA S2.2.4.
Best for: Anyone who wants to understand what the "selective GHRP" label actually means, and where the evidence starts and stops.
Not ideal for: Anyone hoping the selectivity data translates directly into a safety clearance for human self-administration. It does not.
What to look for: When a vendor or influencer cites ipamorelin's cortisol selectivity, ask which species the data came from. The landmark selectivity studies were conducted in rats and swine, not humans.
Decision shortcut: If you compete in any sport governed by the World Anti-Doping Code, ipamorelin is explicitly named on the 2025 WADA Prohibited List under S2.2.4 (Growth Hormone Releasing Factors). The "research peptide" label on the packaging does not create a doping exemption.
What Ipamorelin Actually Is: A Selective GHRP
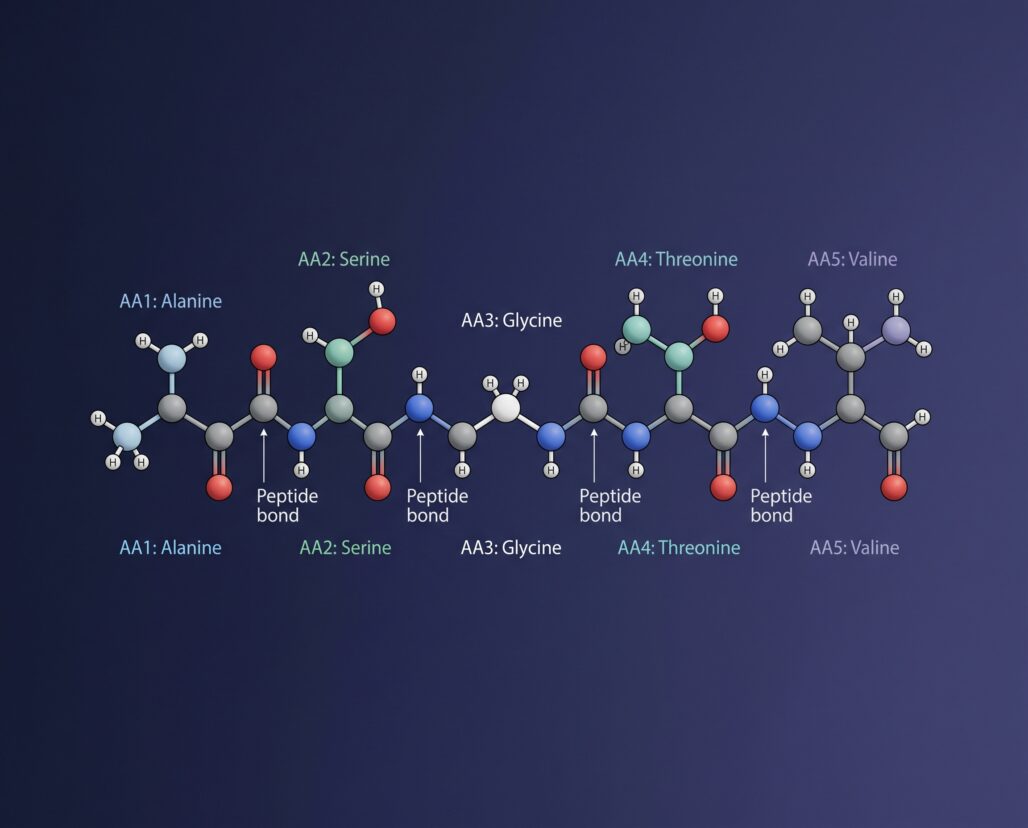
Ipamorelin's formal chemical identity is Aib-His-D-2-Nal-D-Phe-Lys-NH2 — a pentapeptide (five amino acids) incorporating non-natural amino acid residues that improve receptor binding and metabolic stability. It was developed at Novo Nordisk and first characterized in the scientific literature in 1998 by Raun and colleagues in the European Journal of Endocrinology (PMID 9849822).
The compound belongs to the growth hormone secretagogue (GHS) class. GHSs are molecules that stimulate GH release from the pituitary — but they do so by a completely different mechanism than growth-hormone-releasing hormone (GHRH), the body's own GH-release signal. GHSs bind the GHS receptor subtype 1a (GHS-R1a), which is also the receptor for ghrelin, the gut-derived hormone associated with hunger and energy homeostasis. Ipamorelin is, technically, a synthetic ghrelin-receptor agonist: it turns on the same receptor that ghrelin activates, but it was engineered in a laboratory rather than produced by the body.
The "five amino acids" detail is worth noting because it distinguishes ipamorelin structurally from longer peptides in the same class (GHRP-6 is a hexapeptide; GHRP-2 is also a hexapeptide). The shorter, modified chain contributes to its receptor-binding profile — specifically, its ability to activate the GHS-R1a without significantly triggering the secondary receptor pathways responsible for cortisol and prolactin release.
You will see ipamorelin discussed alongside other growth hormone secretagogues when exploring what peptides are and evaluating peptide safety broadly — and the regulatory and evidence questions it carries are similar to those surrounding the rest of that class.
Why "Selective" Matters: The GHRP-2 and GHRP-6 Comparison
The word "selective" does specific work in ipamorelin's pharmacology, and it is worth unpacking carefully rather than accepting it as a blanket quality endorsement.
Older growth hormone-releasing peptides — particularly GHRP-2 and GHRP-6 — activate GHS-R1a effectively, but they also trigger secondary hormonal cascades. In animal studies, GHRP-2 and GHRP-6 produce measurable elevations in ACTH (adrenocorticotropic hormone), cortisol, and prolactin at doses used to stimulate GH. This is a meaningful limitation: cortisol is a catabolic hormone, and chronically elevated cortisol is associated with muscle breakdown, immune suppression, and metabolic disruption. Prolactin elevation carries its own set of effects on reproductive hormones and fluid balance.
The Raun et al. 1998 study (PMID 9849822) tested ipamorelin against GHRP-6 and GHRH in rats and conscious swine. The finding was striking: "ipamorelin is the first GHRP-receptor agonist with a selectivity for GH release similar to that displayed by GHRH." Even at doses 200 times the ED50 for GH release, ipamorelin produced no significant elevations in ACTH, cortisol, FSH, LH, prolactin, or TSH. The study also quantified its GH-release potency: an EC50 of 1.3 nmol/L in vitro and an ED50 of approximately 2.3 nmol/kg in conscious swine, achieving peak plasma GH levels of 65 ng/mL.
This is a genuine pharmacological distinction, not a marketing invention. In head-to-head preclinical comparisons, ipamorelin produces comparable GH elevation to other GHRPs while avoiding their collateral hormonal effects.
The important caveat: every one of those comparisons was conducted in non-human animals. Whether the same selectivity profile holds at the receptor level in humans, at therapeutic doses, in people with varying baseline hormonal status, remains unconfirmed in controlled human trials.
Mechanism: How GHS-R1a Agonism Drives GH Release
GH release from the anterior pituitary is regulated by competing signals. GHRH (from the hypothalamus) drives release; somatostatin inhibits it. Ipamorelin adds a third input by binding GHS-R1a receptors on pituitary somatotroph cells and in the hypothalamus, stimulating GH release through a calcium-dependent signaling cascade.
Ipamorelin appears to potentiate GH pulsatility — the natural pulse-and-trough pattern — rather than producing a flat, prolonged elevation. A 2024 study in Physiology and Behavior (PMID 39043357, Lu et al.) confirmed ipamorelin's GHS-R1a agonism and found it significantly inhibited ileum smooth-muscle contractions (IC50 of 11.7 micromolar), evidence of active peripheral receptor engagement in GI tissue.
GHS-R1a is expressed widely: pituitary, hypothalamus, heart, lung, and GI tract. A 2020 study in the Journal of Experimental Pharmacology (PMID 32801950, Mohammadi et al.) showed that intravenous ipamorelin significantly attenuated colonic hypersensitivity and somatic allodynia in rats, with effects blocked by a GHS-R1a antagonist — confirming receptor specificity. Ipamorelin is not a narrow, pituitary-only drug, which is one reason predicting its full human effect profile requires human data, not animal-model extrapolation alone.
Clinical Trial History: The Post-Operative Ileus Story
Ipamorelin's most advanced clinical development targeted post-operative ileus (POI) — the temporary gut-motility paralysis that follows abdominal surgery. The rationale was direct: GHS-R1a receptors are expressed throughout the GI tract, and GHS agonists accelerate motility recovery in animal surgery models.
Novo Nordisk advanced ipamorelin into early-phase clinical trials for POI. The trials were discontinued. The compound did not reach regulatory approval for POI or any other indication. This history carries two important implications. First, ipamorelin is not completely untested in people — early-phase trials generate human safety and pharmacokinetic data even when unpublished. Second, the compound was evaluated for a specific medical purpose, failed to achieve approval, and was dropped by its originator. The arc from discontinued Novo Nordisk drug candidate to widely sold "research peptide" is the part that demands scrutiny.
Published human data remains thin across the GHS category. A 2020 review in Translational Andrology and Urology (PMID 32257855, Sinha et al.) that examined five GHS compounds including ipamorelin found "a paucity of data examining the clinical effects of these compounds currently limits our understanding of GHS' role in the treatment of men with hypogonadism" — a candid assessment from researchers treating the category favorably.
Regulatory Status: FDA, WADA, and the Research-Peptide Loophole
The regulatory picture for ipamorelin is clear even if the vendor landscape makes it appear murky.
FDA status. Ipamorelin is NOT FDA-approved as a drug, dietary supplement, or compounded medication for human use. It was a clinical-trial-stage drug that was abandoned in its post-operative ileus indication and never received approval. Vendors who sell it as a "research peptide" or "for laboratory use only" are using labeling language to navigate the unapproved drug framework, not to accurately describe the product's intended end use. The FDA has demonstrated willingness to act against peptide vendors using this labeling strategy when products are marketed for therapeutic human use.
WADA status. Ipamorelin is explicitly named on the 2025 WADA Prohibited List under section S2.2.4 (Growth Hormone Releasing Factors, within the broader S2 category: Peptide Hormones, Growth Factors, Related Substances and Mimetics). The full WADA language lists ipamorelin alongside anamorelin, capromorelin, ibutamoren (MK-677), lenomorelin, macimorelin, and tabimorelin as prohibited growth hormone secretagogues. Prohibition is all-times — not limited to the competition window. Any athlete subject to the World Anti-Doping Code who uses ipamorelin, regardless of the "research use" label on the packaging, is committing a doping violation.
The grey market. A 2026 review in Sports Medicine (PMID 41966639, Mendias and Awan) categorized ipamorelin among "prominent approved and unapproved peptides marketed direct to patients," noting that "many unapproved peptides demonstrate favorable tissue repair and metabolic outcomes in animal models, but rigorous human safety data are scarce, and there is potential for serious harm to patients." Grey-market ipamorelin products are manufactured without FDA oversight of purity, sterility, or actual peptide concentration. Independent testing of research-peptide products has repeatedly found significant discrepancies between labeled and actual content. This is not a hypothetical contamination scenario — it is a structural feature of an unregulated supply chain.
Side Effects and What the Risk Profile Actually Looks Like
The framing of ipamorelin as the "safe" GHRP deserves unpacking, because "safer than GHRP-2" and "safe for human use" are different claims.
The selectivity advantage is real, but bounded. The absence of significant cortisol and prolactin elevation in animal studies at pharmacological doses is a genuine pharmacological advantage over GHRP-2 and GHRP-6. It means ipamorelin avoids one class of hormonal side effects that limits older GHRPs. That advantage is documented in non-human models. Whether it translates with the same magnitude to human physiology has not been established in a published, peer-reviewed human trial.
Reported effects in human contexts (limited data). Commonly noted side effects from early-phase trials and grey-market use include injection-site reactions, transient headache, flushing, and lightheadedness — consistent with GHS-R1a vasodilatory signaling. None rises to severe adverse event level based on available early-phase observations, but that observation comes from a narrow evidence base.
Unknowns that matter clinically. Supraphysiologic GH is associated with insulin resistance, edema, carpal tunnel syndrome, and possible cardiovascular remodeling over long periods. Whether ipamorelin drives GH to supraphysiologic levels in humans, at which doses, and with what consequences over months of use is not established by published data. A 2026 review in the American Journal of Sports Medicine (PMID 41476424, Mayfield et al.) confirmed that for ipamorelin plus CJC-1295, "information regarding the indications, dosing, frequency, and duration of treatment remains unknown."
Pregnancy and nursing. No human safety data exists for ipamorelin in pregnant or nursing individuals. The compound activates receptor systems involved in appetite, gut motility, and pituitary hormone signaling — all tightly regulated during pregnancy. Blanket avoidance is the only defensible position, not a precautionary hedge.
Grey-market quality. Products sold without pharmaceutical-grade manufacturing oversight may contain endotoxins, incorrect concentrations, or degraded peptide. The selectivity data says nothing about product purity from an unregulated supply chain.

Frequently Asked Questions
Is ipamorelin safer than GHRP-2 or GHRP-6? In animal pharmacology, yes — the cortisol and prolactin selectivity data is real and peer-reviewed. In terms of human safety, no one can responsibly say one unapproved compound is "safer" than another unapproved compound in human use, because neither has completed the human trials needed to establish a safety profile. The selectivity advantage reduces one category of hormonal concern; it does not eliminate the other unknowns.
Why is ipamorelin usually sold with CJC-1295? CJC-1295 is a GHRH analogue — it activates a different receptor and drives GH release through a different pathway. The combination targets two independent stimulatory inputs to pituitary GH release simultaneously, which produces a larger GH pulse in animal models than either compound alone. For a full comparison of the two compounds and their combined rationale, see our CJC-1295 explained article and the head-to-head CJC-1295 vs ipamorelin comparison.
Does ipamorelin build muscle? Ipamorelin stimulates GH release in animal models, and elevated GH increases IGF-1, which drives protein synthesis. That is the chain of reasoning behind its body-composition use. Direct human evidence for ipamorelin producing measurable lean mass changes in a controlled trial does not exist at a level that supports a clinical claim.
Can I get ipamorelin from a compounding pharmacy? This depends on jurisdiction and changes as regulations evolve. In the United States, the FDA's position on GHS compounds for compounding has tightened in recent years, and ipamorelin's status as a discontinued unapproved drug candidate creates a complicated legal framework. Consult a licensed physician for current, jurisdiction-specific guidance.
What does WADA S2.2.4 mean for recreational athletes? WADA's prohibited list applies to athletes subject to the World Anti-Doping Code. If you compete in any Olympic sport, most professional sports, or sports governed by a national body that adopts the WADA code, the prohibition applies to you. Recreational athletes not subject to testing are not bound by WADA rules, but they are still subject to FDA regulations around unapproved drugs, and the safety unknowns apply regardless of competitive status.
Tracking a protocol like this? Our companion app, StackMyMed, lets you log doses, schedule them, and check interactions across everything you take — alongside, never instead of, your clinician’s guidance.
Conclusion: The Bottom Line on Ipamorelin
Ipamorelin's selectivity profile is a real and meaningful pharmacological characteristic. Among the GHRP class, its ability to stimulate GH release without significant cortisol or prolactin elevation — documented in animal studies by the original Novo Nordisk team — represents a genuine advance over older compounds. That is the honest case for ipamorelin.
The limits of that case are just as real. The clinical trial program that would have established human efficacy and safety in post-operative ileus was discontinued without approval. Published human data from those trials is not available. The GH-pulsatility, body composition, and anti-aging applications that dominate the current marketing conversation have not been studied in controlled human trials. The selectivity advantage does not address the long-term questions around sustained GH elevation in adults, and it says nothing about product quality when purchased from grey-market vendors.
Regulatory status is unambiguous: NOT FDA-approved, explicitly prohibited by WADA, and sold under research-use labeling that serves as a legal workaround rather than a safety guarantee.
If you are evaluating growth hormone secretagogues for a legitimate medical reason — hypogonadism management, recovery from muscle-wasting illness, or clinical research — the conversation belongs with a physician familiar with the current evidence and the compounding pharmacy framework in your jurisdiction. If you are an athlete, the WADA placement ends the conversation regardless of what form it is purchased in.
Next steps:
- Start with the fundamentals: What are peptides? — plain-language explanation of how synthetic peptides are built and classified.
- Understand the regulatory context: Are peptides safe? — covers the full tier structure from FDA-approved compounds to grey-market research chemicals.
- If you are comparing specific GHRH/GHRP combination protocols, CJC-1295 explained covers ipamorelin's most common pairing compound in detail.
- For a direct side-by-side, CJC-1295 vs ipamorelin maps the mechanism, evidence, and risk differences between the two.
This article is for informational purposes and not medical advice. Peptides, especially those marketed for therapeutic use, can interact with medications and health conditions. Consult a licensed physician before starting any supplement, particularly if you are pregnant, nursing, taking prescription medications, or managing a chronic condition.
